Apheresis, Infusion Nursing Teams at the Forefront of Innovation, Compassionate Care
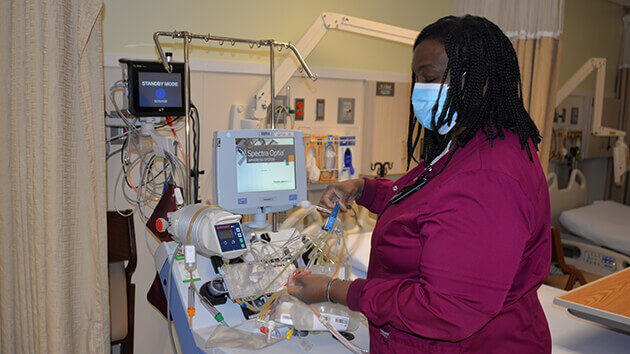
For nearly 20 years, Herma Lee, MS, RN, has treated patients in Albany Medical Center’s Apheresis and Infusion Unit. Over the past two decades, she has delivered numerous treatments to patients from across the region, but what drew her to Albany Medical Center in the first place was her desire to learn.
“Apheresis? I had no idea what it was, and that’s what drew me. I had no idea what it was, but I was going to learn,” Lee said.
She recalled the recruiting event where she interviewed for the position.
“The nurse manager that interviewed me, she was passionate about what she did here in apheresis, and it made me want to be a part of it,” Lee said.
Therapeutic apheresis is a process that separates the components of a patient’s blood using an apheresis machine, allowing certain components to be removed and disposed of while the rest of the blood is re-infused back into the patient. This is used to treat conditions such as sickle cell disease, where a patient receives a red cell exchange to remove the abnormal red blood cells, or acute leukemia, where a patient will receive a white blood cell depletion.
On a daily basis, about two or three nurses are dedicated to apheresis procedures, while other members of the team deliver a range of infusion treatments, from chemotherapy to monoclonal antibody treatment for Crohn’s disease. The apheresis and infusion nursing team also played a significant role in Albany Medical Center’s Covid-19 monoclonal antibody program.
“There’s a lot to learn,” said Johanna Huse, RN, with Albany Medical Center’s Apheresis and Infusion Unit.
Like Lee, Huse saw Albany Medical Center as an educational opportunity. Huse began working at Albany Medical Center after graduating seven years ago, first as a nurse in Neurology for two years before moving to the Apheresis and Infusion Unit.
In addition to administering drugs that are already on the market, the unit will assist with case studies for new medication for the federal Food and Drug Administration (FDA).
“I find it very interesting, especially with the new drugs coming on the market,” Huse said. “We always have something that we’re learning about and having trainings on.”
The opportunity to work with new treatments also appeals to Lorrai Carpenter, RN, lead clinical nurse at the Glens Falls Hospital Infusion Center. She said the Infusion Center sees patients with rare autoimmune and neurological disorders. Several years ago, the department assisted in making Radicava, an intravenous infusion treatment for amyotrophic lateral sclerosis (ALS), available to the local community.
“Being on the cutting edge of treatment, that’s important,” Carpenter said. “It’s all about serving the community.”
Infusion services are offered across the Albany Med Health System. Ruth Jameson, MS, RN, CRNI, nurse manager of the Infusion Center and Vascular Access at Glens Falls Hospital, described the Infusion Center as a close-knit team. Jameson has worked at Glens Falls Hospital for about 27 years, 10 of which have been in the Infusion Center.
“Infusion nursing always interested me,” Jameson said. “I’ve loved IVs from the moment I became a nurse. In the Infusion Center, we have highly skilled staff who continually learn new medications and work with pharmacy to offer these treatments to our community. We created a separate infusion site to offer monoclonal antibody treatments to Covid-19 outpatients, which was challenging and rewarding.”
Every day at the Infusion Center is different. The center offers a wide range of treatments such as intravenous antibiotics, hydration therapy, blood transfusions, as well as specialty medications for various conditions. Since many treatments occur over several weeks or months, Jameson said that patients can become like family.
At Saratoga Hospital, patients can receive infusion therapy such as immunoglobulins and monoclonal antibodies to treat various autoimmune diseases as well as IV hydration, electrolyte replacement, and first dose teaching for self-injectable medications. Katie Waite, RN, BS, IgCN, is a part of a team that treats about 20 patients a day at the Infusion Center.
Waite has worked at Saratoga Hospital for more than 23 years, 14 of which have been in outpatient infusion therapy between the hospital and Malta locations.
Waite said that while infusion therapy may seem intimidating for someone new to the job, several months of training helps prepare staff to treat numerous conditions and learn new medications offered at the infusion center.
“Every day, I’m learning,” Waite said.
She also cited the close connection that the nursing teams form with patients as one of the reasons she enjoys working at the Outpatient Infusion Center.
“I love working here knowing that I’m helping patients maintain quality of life while living with a chronic illness,” Waite said. “We build relationships with our patients, and they become like family.”
Outside the walls of our hospitals, the Albany Med Health System Visiting Nurses brings infusion therapy right to a patient’s own home.
“With Albany Med Health System Visiting Nurses, patients can receive IV medication required to treat their illness while remaining home where most people are most comfortable,” said Visiting Nurses CEO Samantha DiCicco, RN. “This helps to alleviate the stress many feel when admitted to the hospital and can help healing.”
The Visiting Nurses works with each Albany Med Health System campus to get patients back into their own homes, including those that require IV medication. Once the patients are home, Visiting Nurses will help teach patients or their families how to infuse IV medication or hydration as well as work with the patient’s physician to ensure the patient is comfortable to receive their infusion.
“We provide the perfect balance of healing and home,” DiCicco said. “The Albany Med Health System is truly with our patients for everything.”

